A New Care Model: Moving From Remote Patient Monitoring to Remote Patient Care
After reading this article, you will be able to discuss the need for a new care delivery model moving from Remote Patient Monitoring to Remote Patient Care.
SUMMARY:
Remote Patient Monitoring (RPM) provides consistent physiologic measurements.
To date, results of RPM on clinical and cost effectiveness have been mixed.
Although the technology is reliable, a new clinical care model is needed to maximize the potential of RPM
RPM CHALLENGES RESULTING in MIXED OUTCOMES:
Data overload with large volumes of continuous or intermittent data
Lack of patient context of the data
Lack of clinical prioritization
Lack of integration and interoperability with existing systems
Ongoing patient adherence
Digital skills of the patient and ability to use devices
Loss of trust in RPM accuracy
Diminishing likelihood to take appropriate actions
NEED A NEW MODEL:
To drive success, need to shift from RPM as a technology tool to a mode of true care transformation and delivery.
Need to shift focus toward a team-based, protocol-driven program providing total care
Patient Risk Stratification becomes critical.
Consider readmission and clinical deterioration likelihood
Not everyone needs to be remotely monitored/cared for
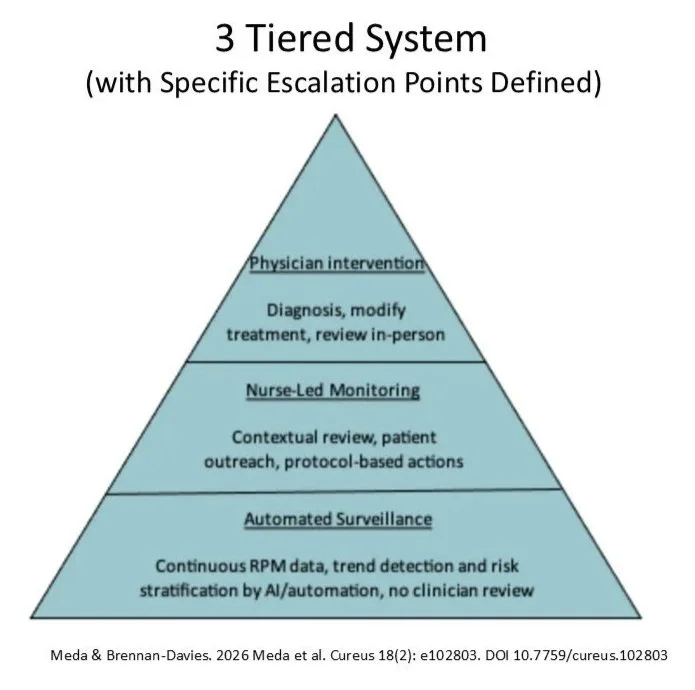
The New Model: An Inter-collaborative Team
Designed to provide comprehensive integrated strategies to provide coordinated patient management, improve outcomes, and decrease costs.
Patient Centric
Dynamic process
Action steps at each tier of the model
Clear escalation points from predefined clinical thresholds or demonstrate concerning trajectories
Who provides the care and when?
What is the staffing model?
How is the team workforce managed?
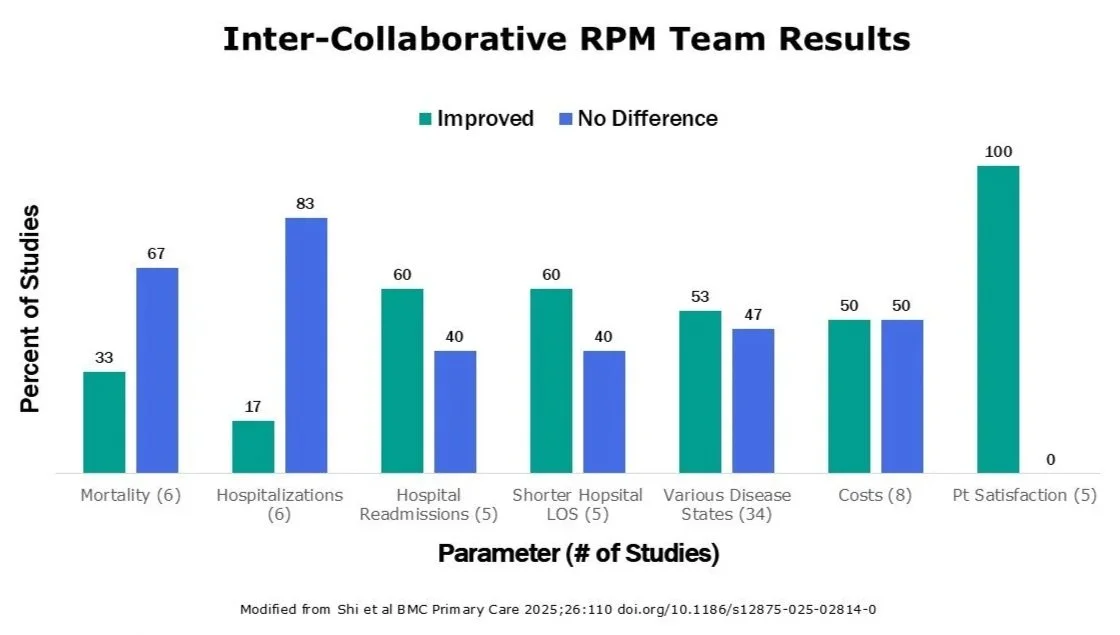
Various reports document the benefits of an outpatient Inter-Collaborative Team Care with inconsistent results:
CONCLUSIONS:
RPM can be used for a variety of chronic outpatient conditions, driving patient engagement and self-care.
RPM has produced inconsistent clinical and economic results in real clinical practice.
The issue is not the technology but rather the level of clinical interpretation and care delivery.
A new care model is needed to move from Remote Patient Monitoring to Remote Patient Care involving an Inter-Collaborative Team.
Use of RPM has rapidly expanded, providing a potential safety net.
Despite this promised performance, RPM has resulted in inconsistent outcomes (clinical and financial).
The issue is not the technology perse, but rather the care delivery model.
A new Inter-Collaborative team model is needed with a patient-centric approach of care delivery.
Supporting patient self-management of multiple chronic diseases over a lifetime is a significant challenge.
Let’s have a brief chat to optimize your RPM program.